Loading...
tech#diabetic foot ulcers#Siren Socks review#Sensoria smart socks
Step Into the Future: A Hands-On Review of Siren Socks and Sensoria for Diabetic Foot Health
Blood Sugar Control
April 3, 20268 min read
The High-Tech Fight Against the 'Silent' Ulcer
I remember the first time I realized my feet were no longer "mine." It wasn't a sudden pain; it was the absence of it. I had stepped on a small Lego piece in my living room, and it wasn't until I saw a red smudge on the carpet that I realized I was bleeding. Like millions of others living with diabetes, I struggle with peripheral neuropathy—a condition where high blood sugar damages the nerves in the extremities. For years, my morning routine involved a mirror, a flashlight, and a deep sense of anxiety as I performed manual foot checks, searching for a blister or a red mark I couldn't feel.
Foot ulcers are the "silent" enemy of the diabetic community. They are the leading cause of diabetes-related hospitalizations and, tragically, the primary precursor to lower-limb amputations. But here is the secret the medical community has known for years: ulcers don't just appear out of nowhere. They are preceded by inflammation. Long before the skin breaks, the tissue becomes inflamed, and that inflammation shows up as heat. This "pre-ulcer" state is our window of opportunity.
If we can catch a "hot spot"—an area just a few degrees warmer than the surrounding tissue—we can stop an ulcer before it even begins. This is where "Smart Footwear" enters the fray. No longer just pieces of fabric, these devices act as 24/7 guardians, using medical-grade sensors to do what our damaged nerves cannot: tell us when our feet are in danger.
Siren Socks: The Temperature-Sensing Revolution
When I first received my Siren Socks, I expected something bulky or "medical" looking. I was pleasantly surprised. The unboxing experience felt more like receiving a high-end pair of athletic socks than a clinical device. The fabric is a soft, moisture-wicking blend that feels substantial but not thick enough to crowd your shoes.

The magic of the Siren system lies in its "Neurofabric." Embedded directly into the weave are six microsensors positioned at the most common pressure points: the heel, the ball of the foot, the big toe, and the outer midfoot. Unlike older technologies that required bulky inserts, these sensors are invisible to the touch. You don't feel them when you walk, and there are no wires to poke or prodded your skin.

How does it work in practice? The socks communicate via Bluetooth to the Siren App. The system establishes a "baseline" for your feet. Every time you put them on, the app compares the temperature of your left foot to your right foot. If a specific spot on your right big toe is significantly warmer than your left, the app sends a push notification: "Hot spot detected."
But Siren doesn't stop at an app alert. One of the most reassuring features for someone with high-risk feet is the clinical back-end. Siren operates on a Remote Patient Monitoring (RPM) model. This means your data isn't just sitting on your phone; it’s being monitored by a licensed nurse at Siren’s headquarters. If a persistent hot spot is detected, a real human—a professional—calls you to walk through the next steps, whether that’s offloading weight, checking for a foreign object, or scheduling an immediate appointment with your podiatrist.
Sensoria: Beyond Temperature with Pressure Mapping
While Siren focuses on the result of friction (heat), Sensoria focuses on the cause of friction (pressure and gait). I’ve always been an active person, and as a diabetic, I’m constantly told that walking is the best medicine—but it’s also the biggest risk. Sensoria is designed for the active diabetic who wants to understand exactly how their feet are hitting the pavement.

The Sensoria system uses textile pressure sensors located under the plantar area. The "brain" of the operation is the Sensoria Smart Core, a small, lightweight device that snaps onto the ankle of the sock. It tracks more than just steps; it monitors your cadence, your impact force, and your foot landing technique (whether you are a heel striker or a forefoot striker).
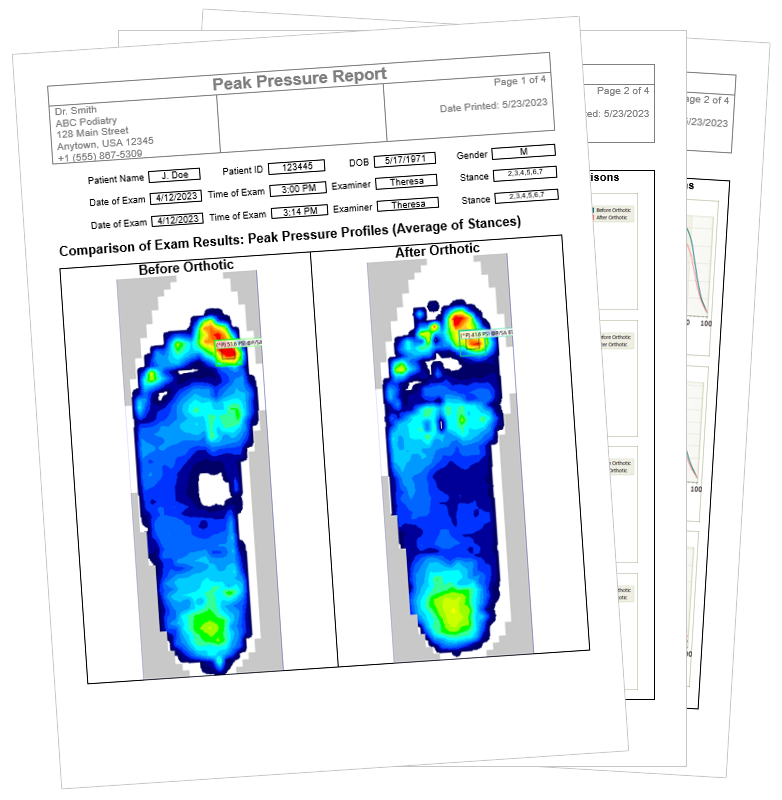
For a runner or a power-walker with diabetes, this is a game-changer. The Sensoria Walk app provides real-time biofeedback. If you start to favor one side or if your impact force becomes too high—increasing the risk of a "charcot foot" or a pressure ulcer—the app provides an auditory cue. It’s like having a physical therapist whispering in your ear, telling you to shorten your stride or adjust your posture to protect your feet.
Head-to-Head: Comfort, Durability, and Daily Life
Putting these through the "Laundry Test" was my biggest concern. We’re talking about high-tech electronics, after all. Siren socks are surprisingly hardy; they are machine washable and can be dried on low heat. However, they have a limited lifespan (usually a few months of continuous wear) before the sensors lose calibration, which is why their subscription model regularly sends you fresh pairs. Sensoria socks are also washable, but you must remember to snap off the Smart Core device first.

In terms of connectivity, both use Bluetooth Low Energy (BLE). I found Siren to be more "set it and forget it." You put the socks on, and they just work. Sensoria requires a bit more interaction—snapping on the core and starting a "session" in the app if you want the detailed gait analysis.
Battery Life:
- Siren: The batteries are built into the socks and last for the life of the garment (about 4–6 months). No charging required.
- Sensoria: The Smart Core is rechargeable via USB and typically lasts for several days of active use.
Style and Fit: Both brands have done an excellent job of making these look like normal socks. I was able to wear both with my custom orthotics and my standard New Balance walking shoes without any tightness. Siren feels more like a dress sock or a standard crew sock, while Sensoria has a more "athletic compression" feel.
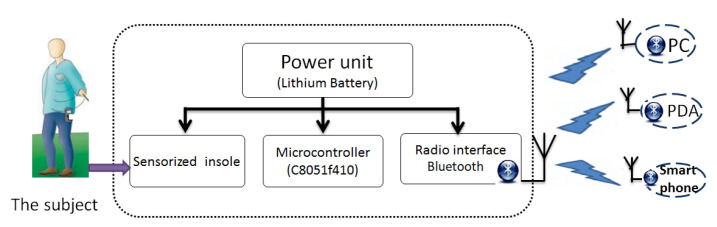
Data-Driven Peace of Mind: Why Tech Beats Manual Checks
The traditional "hand-check" method is flawed. Research shows that the human hand can only detect temperature differences of about 2 to 3 degrees Celsius, and even then, it’s highly subjective. By the time your foot feels "hot" to your hand, the inflammation is already well underway. Smart socks can detect changes as small as 0.1 degrees.
This shift to Remote Patient Monitoring (RPM) is fundamentally changing the doctor-patient relationship. Instead of waiting for a quarterly check-up to tell my podiatrist, "I think my foot felt weird last Tuesday," I can provide a digital log of every temperature spike over the last 90 days. It turns "scary" data into actionable health choices.
When my Siren app alerted me to a hot spot last month, I didn't panic. I followed the protocol:
- I sat down and rested.
- I inspected the area with a mirror (no break in the skin yet!).
- I switched to a wider pair of shoes for the next two days.
- The "heat" dissipated, and a potential ulcer was avoided.
The Verdict: Which Smart Sock is Right for You?
Choosing between these two depends entirely on your risk level and lifestyle.
Best for High-Risk Patients: Siren Socks
If you have a history of ulcers, significant neuropathy, or struggle to perform daily foot checks, Siren is the gold standard. The combination of 24/7 temperature monitoring and the "safety net" of a remote nursing team provides a level of security that is worth every penny. It is a medical tool designed for prevention.
Best for the Active Diabetic: Sensoria
If your primary goal is to stay active while minimizing risk, Sensoria is the winner. Its ability to analyze how you move and provide real-time feedback on gait and pressure is invaluable for runners and walkers. It’s more of a "performance" tool that happens to have incredible safety benefits for diabetics.

The future of diabetic foot health is incredibly bright. We are moving toward a world where smart insoles and even integrated "smart shoes" will be the norm. For those of us living with "sugar feet," this technology isn't just a gadget—it's mobility, it's independence, and it's peace of mind.
My Final Thought: Don't wait for a wound to start caring for your feet. Whether you choose Siren, Sensoria, or simply commit to more rigorous manual checks, remember that your feet carry you through the world. They deserve the best protection technology can offer.
Have you tried smart socks or other diabetic wearables? Share your experience in the comments below, or sign up for our newsletter for the latest reviews on blood sugar management tech!